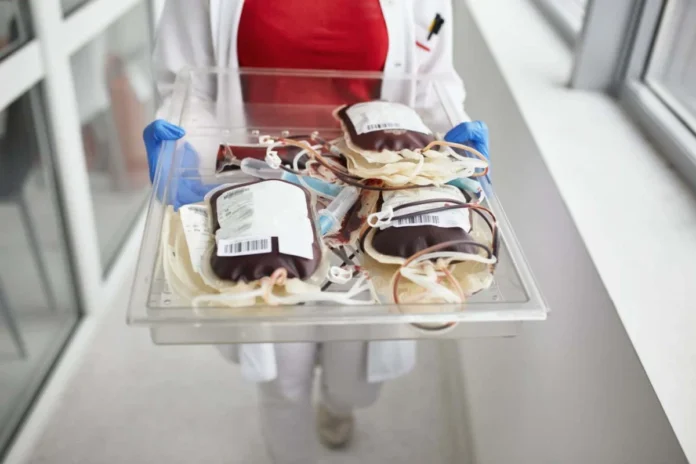
A growing number of patients are making a startling and potentially dangerous request: that their blood transfusions come from donors who have not been vaccinated against COVID-19. This trend, fueled by a surge of misinformation surrounding vaccine safety, is creating significant logistical challenges for healthcare providers and, in some cases, leading to life-threatening delays in critical medical treatments. Medical professionals are grappling with how to address these unfounded fears while ensuring timely and safe patient care.
The Rise of Vaccine-Specific Blood Requests
The phenomenon has been most acutely observed in the United States, where at least one major medical center has been forced to accommodate these unusual demands. Vanderbilt University Medical Center in Nashville, Tennessee, has reported instances where patients or their caregivers have explicitly requested directed blood donations – where the blood comes from a specifically chosen individual, often a relative or friend, rather than the general blood supply. The crucial, and concerning, criterion for these requests is the donor’s COVID-19 vaccination status.
Dr. Jeremy Jacobs, a physician at Vanderbilt University Medical Center, highlighted the root cause of these requests: "These requests were often driven by misinformation about vaccine safety and the blood supply, rather than evidence-based transfusion concerns." He emphasized the critical point that "the community blood supply is already highly regulated and carefully screened, and there is no evidence that requesting unvaccinated blood improves transfusion safety."
Data and Scope of the Issue
A study conducted by Dr. Jacobs and his colleagues at Vanderbilt analyzed blood donation records and patient requests between January 2024 and December 2025. Their findings revealed that 15 patients, or their representatives, specifically asked for directed donations to ensure the blood came from an unvaccinated donor. This number, while seemingly small in the context of a large medical center, represents a significant deviation from standard transfusion protocols and points to a broader societal concern rooted in vaccine hesitancy.
While directed donations are a standard practice in some situations, such as for patients with rare blood types, their use for general transfusion purposes is often discouraged due to operational complexities and potential risks. In countries like the United Kingdom and Australia, directed donations are typically only permitted under exceptional circumstances. In the U.S., policies vary, but the practice is generally allowed though not preferred, with blood banks not recording or disclosing the vaccination status of anonymized donors.
The Perilous Impact of Delays
The consequences of these vaccine-specific blood requests can be severe, primarily due to the delays they inevitably cause. In the most alarming case reported by Vanderbilt, a patient’s hemoglobin levels dropped to a critical point, a condition that can lead to severe organ damage and failure, solely because the necessary transfusion was postponed while a suitable unvaccinated donor was sought. Another patient developed anemia as a direct result of these avoidable delays.
"Directed donation is operationally more complex than using the routine blood supply," Dr. Jacobs explained. "It requires additional coordination, collection, processing, tracking and timing." This added complexity diverts valuable resources and time away from standard, efficient blood transfusion processes, potentially impacting the availability of blood for other patients in urgent need.
Understanding Directed Donations and Their Risks
Historically, directed donations saw an increase during the HIV/AIDS epidemic in the 1980s and early 1990s, as individuals sought greater assurance of blood safety. However, the current trend is distinct, driven by specific anxieties about COVID-19 vaccines.
It is important to note that directed donations, while seemingly offering more control, can carry their own risks. Unlike the community blood supply, which often comprises donations from repeat, regular donors who may be more accustomed to rigorous screening and may have a history with the blood bank, directed donations can be one-off events. This lack of a consistent donor pool could potentially lead to a higher risk of transmitting infections, although all donated blood undergoes extensive screening.
The Pervasive Nature of Vaccine Misinformation
The requests for unvaccinated blood are intrinsically linked to the pervasive spread of misinformation surrounding COVID-19 vaccines. Despite overwhelming scientific consensus on their safety and efficacy, conspiracy theories have proliferated online and in various communities. These unfounded claims include links to fertility problems, DNA alteration, and even the presence of microchips.
The mRNA COVID-19 vaccines, which involve introducing a small piece of SARS-CoV-2’s genetic code to trigger an immune response, have been subjected to intense scrutiny and, unfortunately, widespread misinformation. Reputable scientific bodies and health organizations worldwide have repeatedly affirmed that these vaccines are safe and highly effective at preventing severe illness, hospitalization, and death from COVID-19. Studies, including one published in 2025, have confirmed the safety of transfusing blood from vaccinated individuals, finding no adverse effects related to the vaccination status of the donor.
Broader Implications and Official Responses
The issue is not confined to the United States. In the UK, the Welsh Blood Service has acknowledged receiving inquiries about the vaccination status of blood donors. Furthermore, a petition was submitted to the UK government requesting the segregation of blood donations based on vaccination status, though it was ultimately rejected.
The trend has even reached legislative levels. In Oklahoma, lawmakers have proposed legislation that would mandate hospitals provide patients with access to blood from unvaccinated donors. Such proposals, driven by public demand, highlight the challenge policymakers and healthcare systems face in balancing patient autonomy with evidence-based medical practice and the efficient allocation of resources.
Expert Analysis and the Path Forward
Ash Toye from the University of Bristol in the UK commented on the situation, stating, "Requests for unvaccinated blood reflect broader uncertainty about vaccines among a proportion of the public, rather than any recognised transfusion risk." This underscores that the core of the problem lies in public perception and the need for effective communication and education.
Dr. Jacobs concluded by emphasizing the dual challenge: "These requests illustrate how misinformation can create real operational burdens for patients, hospitals and blood providers. At the same time, they underscore the importance of addressing patients’ concerns respectfully and thoughtfully, even when those concerns are not supported by evidence."
Moving forward, healthcare providers and public health officials face the critical task of not only ensuring the safety and efficiency of the blood supply but also of actively combating misinformation. This involves transparent communication about blood screening processes, reiterating the safety of COVID-19 vaccines, and providing compassionate, evidence-based guidance to patients who may be experiencing anxiety fueled by inaccurate information. The goal is to maintain public trust in the healthcare system and its life-saving interventions, ensuring that medical needs are met without succumbing to scientifically unsubstantiated fears.